Fistula Treatment
Fistula Treatment in Pune, Kolhapur, Aurangabad – Dr Girish Bapat
FISTULA
An anal fistula is an abnormal tunnel-like passage that forms between the inside of the anus or rectum and the skin around the anus due to an infection or abscess. It leads to pain, drainage, and discomfort. Treatment often involves surgical removal. It is more common in men .
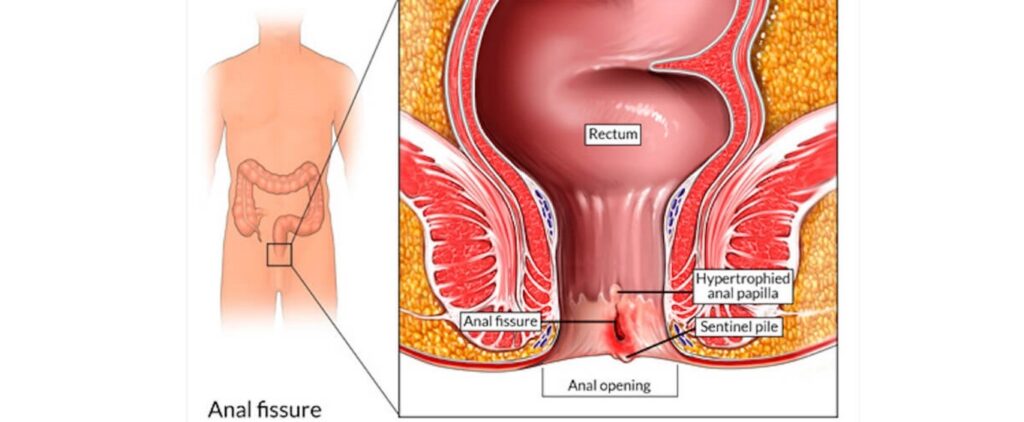
An anal fistula is an abnormal channel between the anal canal (back passage) and the skin around the anal opening. It is associated with an abscess formation around the anus and is more common in men.
Aetiology and Risk Factors
The formation of an anal fistula typically occurs as a result of an anal abscess. About 25-50% of people with an anal abscess will develop an anal fistula. In rare cases, anorectal cancer can occasionally present with an anal fistula.
Another risk factors include:
- Inflammatory bowel disease including Crohn’s disease and ulcerative colitis
- Systemic diseases like tuberculosis, diabetes and HIV
- Past trauma to the anal region
- Past radiation therapy to the anal region
Clinical Features:
Anal fistula commonly occur in cases of chronic anal infection (e.g. anal abscess). They often present with an intermittent or continuous discharge of pus, mucus (slime) or blood on the skin around the anus.
Fistulas may also cause severe pain, swelling, change in bowel habit and systemic features of infection like fever, malaise, weakness.
On examination, an external opening on the skin may be seen; these can be fully open or covered in granulation tissue. A fibrous tract might be felt below the skin on digital rectal examination.
Investigations:
- Rigid sigmoidoscopy can be used to visualize the opening of the tract in the anal canal. Further investigations, such as
- MRI imaging,
- Fistulography
- Endo-anal ultrasound may be used to visualize the remaining part of the tract.
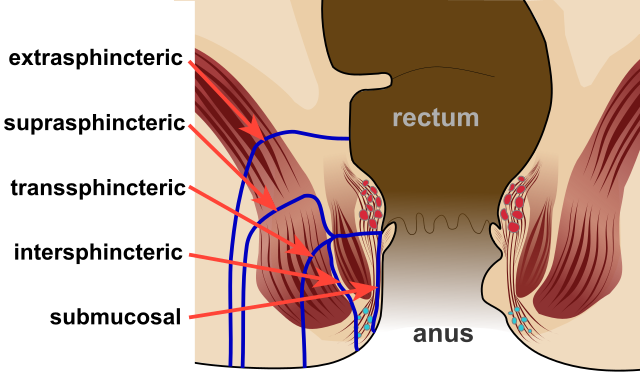
Based on Park’s classification system, there are four types of anal fistulae (Fig):
- Inter-sphincteric fistula (most common)
- Trans-sphincteric fistula
- Supra-sphincteric fistula (least common)
- Extra-sphincteric fistula
Fistula Treatment:
conservative approach can be used in case patient has no symptoms. Various surgical options are available for those deemed not suitable for conservative approach.
Surgical Treatment:
Surgical treatment depends on the Type and Level of Fistula
- Fistulotomy involves laying open of the tract and allowing it to heal by secondary intention. A probe is passed into the tract and the skin, subcutaneous tissue, and internal sphincter are divided in turn, thus opening the tract.
- Placement of a seton (Silk or Nylon) : Pass the seton through the fistula tract around the deep external sphincter after opening the skin, subcutaneous tissue, internal sphincter muscle, and subcutaneous external sphincter muscle. The seton is tightened down and secured with a separate silk tie.
With time, fibrosis occurs above the seton as it gradually cuts through the sphincter muscles and essentially exteriorizes the tract. The seton is tightened on subsequent office visits until it is pulled through over 6-8 weeks. Also it is possible to use cutting seton without associated fistulotomy.
- Other Treatments: Mucosal Advancement Flap, LIFT Procedure, Diversion.
Complications:
Delayed postoperative complications may include the following:
- Recurrence: Standard fistulotomy – The reported rate of recurrence is 0-18%, Seton use – The reported rate of recurrence is 0-17%,
- Incontinence (stool)
- Anal stenosis – The curing process causes fibrosis of the anal canal; bulking agents for stool helps to prevent narrowing
- Delayed wound healing – Usually healing process takes 12 weeks unless an underlying disease process is present (i.e, recurrence, Crohn disease)
TREATMENT FOR FISTULA:
- Hygiene: Keep the anal area clean and dry to prevent infection. Gently clean with mild soap and water after bowel movements.
- Diet: A high-fibre diet with fruits, vegetables, whole grains, and legumes can help prevent constipation and promote regular bowel movements.
- Hydration: Drink plenty of water to maintain soft stools and prevent dehydration.
- Regular Bowel Movements: Respond promptly to the urge to have a bowel movement to avoid straining.
- Avoid Straining: Straining during bowel movements can worsen the condition. Stool softeners can help prevent this.
- Avoid Irritants: Avoid using harsh soaps, scented products, or irritating substances on the anal area.
- Follow Medical Advice: Adhere to any post-surgery or post-treatment instructions provided by General Surgeon in Pune.
- Fistulotomy: This procedure involves cutting open and removing the entire fistula tract. It is often used for simple or low-risk fistulas.
- Advancement Flap: Tissue is moved from the rectum to cover the internal opening of the fistula. This method is suitable for complex or high-risk fistulas.
- Seton Placement: A thin piece of material (seton) is inserted into the fistula to help it heal gradually over time. This is useful for complex or deep fistulas.
F.A.Q
Diagnosing a fistula typically involves these steps:
- Physical Examination: A doctor examines the anal area to look for signs of an opening, drainage, swelling, and other symptoms.
- Probing: A thin instrument is used to gently probe the fistula tract to determine its extent and direction.
- Imaging: Imaging tests like MRI, ultrasound, or fistulography might be used to visualize the fistula’s path and its relation to surrounding structures.
- Assessment: The type, location, and complexity of the fistula are assessed to determine the best treatment approach.
Certain factors can increase the risk of developing an anal fistula. These include:
- Anal Abscess: Having a previous anal abscess increases the risk of a fistula forming.
- Inflammatory Bowel Disease (IBD): Conditions like Crohn’s disease or ulcerative colitis can increase the likelihood of developing anal fistulas.
- Anal Infections: Infections in the anal glands or surrounding tissue can lead to fistula formation.
- Injury or Trauma: Previous injury or trauma to the anal area can contribute to fistula development.
- Crohn’s Disease: This inflammatory bowel disease often involves the anal area and is associated with a higher risk of fistulas.
- Obesity: Excess weight and pressure on the pelvic area can increase the risk of developing anal fistulas.
- Poor Hygiene: Inadequate anal hygiene can lead to infections that might result in fistulas.
- Certain Medications: Medications that suppress the immune system can increase susceptibility to infections.
- Gender: Men are generally more prone to developing anal fistulas than women.